Discover How All-on-4 Implants Differ in Bone Grafting Needs
Missing teeth and jawbone loss can undermine implant success before you even begin, but understanding how bone grafting requirements vary between All-on-4 and traditional dental implants empowers you to choose the best solution. In this guide, you’ll discover why jawbone density matters, when grafting is necessary, and how innovative All-on-4 placement often eliminates or reduces grafting procedures. We’ll compare types of bone grafts, walk through procedural steps, highlight recovery timelines, explore cost considerations, and outline patient suitability in Tulsa, OK. Whether you’re anxious about surgery or budgeting for treatment, you’ll gain clarity on how bone grafting differs in All-on-4 implants versus standard dental implants—and how Tulsa Time Dental Design can support you every step of the way.
What Are Dental Implants and Why Is Jawbone Health Important?
Dental implants replace missing teeth by anchoring titanium posts into the jawbone. This restorative procedure not only restores chewing function and speech but also preserves facial structure by stimulating bone through osseointegration. Healthy jawbone density supplies the stability implants need to integrate, preventing complications like implant loosening or failure. Losing bone volume—often from tooth loss or periodontal disease—compromises implant support and may necessitate bone grafting to rebuild adequate foundation.
Jawbone density matters because implants transfer biting forces into bone, prompting remodeling and strengthening. Without sufficient volume, implants risk micromovement and poor integration. Maintaining or restoring bone health ensures long-term implant success and a confident smile.
Dental Implants and Bone Health: Impact on Jawbone Density and Structure
This review highlights that dental implants are crucial for tooth replacement, with osseointegration being key to their success. It notes that implants generally support bone preservation and can stimulate local bone density, although vigilance is needed for potential complications like peri-implantitis and bone resorption.This research supports the article's explanation of why jawbone density is vital for dental implant success and how implants interact with bone health.
What Defines Standard Dental Implants?
Standard dental implants involve inserting one or more titanium posts vertically into available jawbone. After placement, a healing period allows osseointegration to occur before attaching the final restoration. Key attributes of traditional implants:
Individual post placement matching single- or multi-tooth loss
Healing time of 3–6 months before final crown or bridge
Often requires bone grafting if bone height or width is inadequate
This conventional approach offers versatility for single-tooth replacement but can require extensive grafting when bone loss is present, adding complexity and recovery time.
What Are All-on-4 Dental Implants?
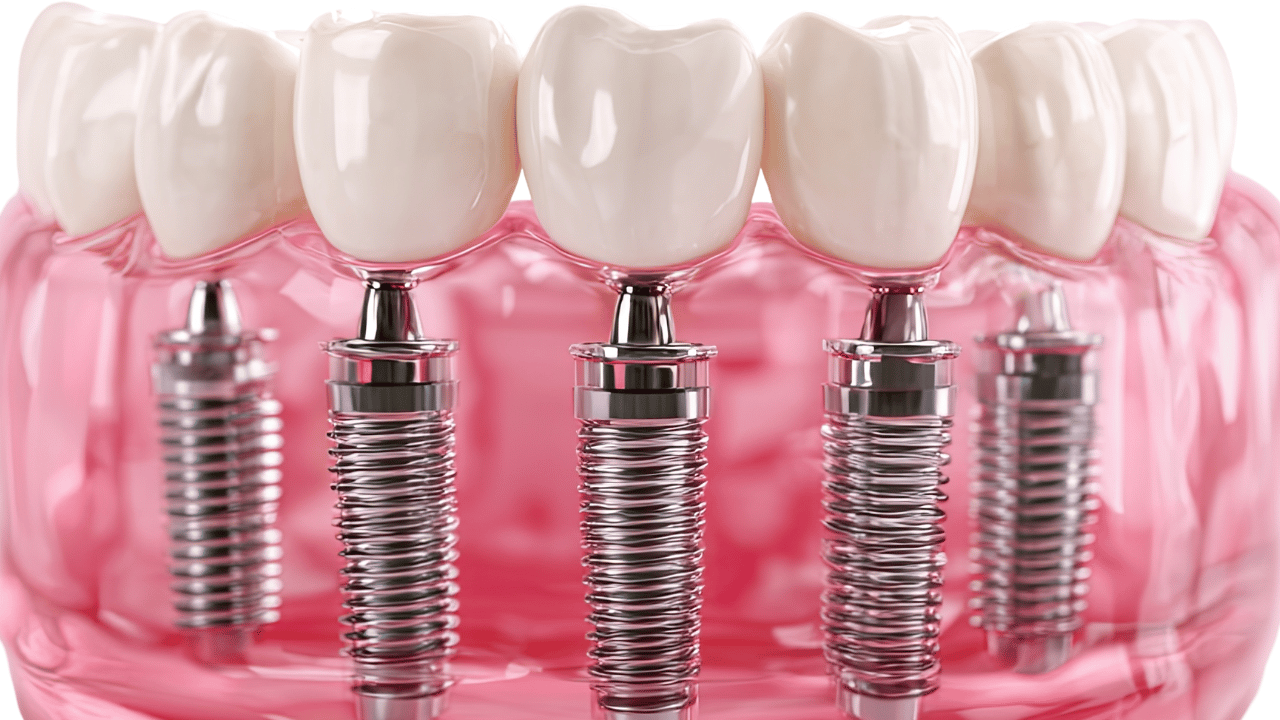
All-on-4 implants restore a full arch of teeth using just four strategically placed posts. Two implants are vertical at the front, two angulated in the back, maximizing contact with dense bone. This protocol enables immediate provisional teeth on the same day as surgery and often avoids bone grafting altogether. The unique features include:
Four posts supporting a fixed full-arch prosthesis
Angled placement to utilize existing cortical bone
Immediate loading to restore function and aesthetics quickly
By leveraging angled implants, this technique bypasses areas of bone deficiency and accelerates treatment for patients with moderate bone loss.
How Does Jawbone Density Affect Implant Success?
Jawbone density directly influences osseointegration, the process by which bone fuses to the implant surface. Low density increases the risk of implant micromotion and failure. Key points:
Bone loss from missing teeth or gum disease reduces volume and strength.
Adequate density provides mechanical stability and long-term support.
Areas like the posterior maxilla often require sinus lifts or grafts before vertical implants.
When bone density is insufficient, grafting builds new bone or reinforces existing structure, enhancing the probability of successful implant integration.
When Is Bone Grafting Necessary for Standard Dental Implants?
Bone grafting becomes necessary when native jawbone lacks the height, width, or density to secure traditional implants. Rebuilding the ridge through grafts ensures stable implant placement and predictable outcomes. Common indications include narrow ridges, deficient alveolar height, and proximity to anatomical structures like the sinus cavity.
What Types of Bone Grafts Are Used in Dental Procedures?
Dental bone grafts utilize different materials to restore jaw volume. The four primary graft types:
Autograft uses your own bone, typically harvested from the chin or hip.
Allograft uses processed human donor bone from tissue banks.
Xenograft uses bovine or porcine-derived bone minerals.
Alloplast uses synthetic biocompatible materials like calcium phosphate.
Each graft type varies in remodeling speed, osteogenic potential, and availability, offering options to match patient preference and clinical needs.
Advances in Bone Grafting Techniques for Dental Implants: A Comprehensive Review
This comprehensive review details various bone graft materials, including autografts, allografts, xenografts, and alloplasts, evaluating their benefits and limitations. It also discusses different grafting procedures like guided bone regeneration, sinus lifts, and socket preservation, which are essential when native bone volume is insufficient for implant integration.This review provides foundational information on the types of bone grafts and the procedures involved, directly supporting the article's sections on bone grafting for standard dental implants.
How Is Bone Grafting Performed for Standard Implants?
Socket Preservation: After extraction, graft material is placed into the empty socket to prevent resorption.
Ridge Augmentation: Grafting substance is attached to the ridge using barrier membranes, increasing bone width or height.
Sinus Lift: For upper back teeth, the sinus membrane is elevated and graft material inserted underneath to gain vertical height.
These surgical steps ensure a solid foundation for vertical implant placement but extend treatment timelines.
What Is the Recovery Timeline After Bone Grafting?
Bone graft healing progresses over three phases:
Initial Healing (0–2 weeks): Soft tissue closure and early inflammation subside.
Osteogenesis Phase (2–6 months): New bone formation within graft material.
Maturation Phase (6–12 months): Remodeling and integration of graft into native bone.
Patients can expect mild swelling and discomfort initially, with dietary modifications and oral hygiene measures critical for success. Implant placement typically follows once adequate bone volume and quality are confirmed on imaging.
What Are the Risks and Complications of Bone Grafting?
Bone grafting risks include infection, graft rejection, and sinus membrane perforation in sinus lifts. Common complications and management:
Infection: Controlled with antibiotics and sterile technique.
Graft Failure: Rare with proper planning; may require revision graft.
Nerve Injury: Uncommon in ridge augmentation but monitored to prevent sensation changes.
Understanding these factors helps you anticipate care steps and work with your provider to minimize complications.
How Do All-on-4 Implants Minimize Bone Grafting Needs?
All-on-4 implants reduce or eliminate grafting by strategically placing angled implants into denser regions of the jaw, such as the anterior ridge. This technique avoids areas affected by atrophy or pneumatized sinuses, offering reliable support without added procedures.
The All-on-Four Treatment Concept: Systematic Review
This systematic review examines the All-on-4 treatment concept, noting its effectiveness in rehabilitating atrophic jaws by maximizing existing bone and often avoiding regenerative procedures. It reports high implant survival rates, indicating a predictable solution for full-arch rehabilitation with immediate function.This systematic review supports the article's claims regarding how All-on-4 implants minimize bone grafting needs and offer high success rates by strategically utilizing available bone.
How Does Angled Implant Placement Reduce Bone Graft Requirements?
By tilting posterior implants at approximately 30–45 degrees, All-on-4 accesses thicker cortical bone beyond the sinus cavity and nerve canals.
Bypasses deficient bone zones
Maximizes bone-to-implant contact
Ensures primary stability without additional grafting
The angled trajectory transforms limited bone volume into a stable anchor for a full-arch prosthesis, streamlining treatment.
When Might Bone Grafting Still Be Needed with All-on-4?
In severe atrophy cases where even anterior bone is compromised, supplemental grafting or zygomatic implants may be considered. Specific scenarios include:
Extremely narrow anterior ridges with limited width
Previous trauma or pathology reducing basal bone volume
Requirement for long-term structural support in complex reconstructive cases
However, most patients with moderate bone loss avoid grafting altogether with All-on-4.
What Are the Benefits of All-on-4 Implants Compared to Standard Options?
Immediate provisional teeth for same-day function
Fewer implants, reducing surgical sites and cost
Minimized need for bone grafts and related procedures
High long-term success rates, often exceeding 95% at five years
These benefits translate into shorter treatment times, less postoperative discomfort, and predictable restorative outcomes for patients facing full-arch rehabilitation.
How Do Bone Grafting Requirements Differ Between All-on-4 and Traditional Implants?
Traditional implants frequently require bone grafts to build vertical or horizontal dimensions, whereas All-on-4’s tilt-driven placement leverages remaining cortical bone. This key distinction reduces surgical interventions and overall treatment duration.
How Do Procedure Complexity and Recovery Times Compare?
Standard implant protocols can span two procedures—graft placement then implant insertion—extending the timeline to 9–12 months. All-on-4 combines extraction, implant placement, and provisional prosthesis in one appointment, with recovery consolidated into a 3–6 month osseointegration phase.
What Are the Cost Differences Related to Bone Grafting for Both Implant Types?
Bone graft materials, additional surgery time, and extended chair visits add 20–40% to the overall cost of standard implant treatments. In contrast, All-on-4’s graft avoidance and single-stage approach typically lower total investment and reduce follow-up appointments.
Who Are Ideal Candidates for Each Implant Type Based on Bone Health?
Standard Implants: Patients with good native bone volume or willing to undergo grafting. Ideal for single-tooth or small-span restorations.
All-on-4 Implants: Patients needing full-arch replacement with moderate bone loss seeking faster results and fewer surgeries.
Assessment of bone volume, overall health, and treatment goals informs candidacy for either solution.
How Can Patients Assess Their Bone Health and Implant Candidacy in Tulsa?
What Diagnostic Tools Are Used to Measure Jawbone Density?
3D cone beam computed tomography (CBCT) and digital panoramic X-rays provide high-resolution images of bone volume and quality. These tools:
Map bone height and width
Identify anatomical landmarks and sinus positions
Quantify bone density values for implant planning
Accurate imaging ensures personalized grafting decisions or All-on-4 placement strategies.
Are There Alternatives to Bone Grafting for Implant Candidates?
In cases of severe atrophy, other graftless options include:
Zygomatic Implants: Longer posts anchoring into cheekbone for upper-arch support.
Pterygoid Implants: Posterior implants engaging pterygoid plate in the skull.
Subperiosteal Implants: Custom frameworks resting on bone surface for extensive atrophy.
These alternatives, like All-on-4, strive to circumvent grafting by utilizing dense anatomical structures.
How Does Tulsa Time Dental Design Support Patients With Dental Anxiety?
Our Tulsa practice combines sedation dentistry, noise-cancelling headphones, warm blankets, and compassionate chair-side manner to ease anxiety. Experienced providers walk you through each step, fostering trust and comfort from consultation to final restoration.
What Financing Options Are Available for Implants and Bone Grafting?
Flexible payment plans, third-party financing, and in-house membership savings enable patients to invest in oral health without financial strain. Tulsa Time Dental Design’s team crafts customized financing solutions so treatment aligns with your budget and timeline.
What Should You Expect During the Bone Grafting and Implant Process?
What Are the Step-by-Step Procedures for Bone Grafting and Implant Placement?
Consultation & Imaging: Clinical exam, CBCT scan, treatment plan discussion.
Grafting Stage (if needed): Harvest or place graft material, secure barrier membranes.
Healing Period: Monitor graft maturation with follow-up visits.
Implant Surgery: Place implants into grafted or native bone under sedation.
Provisional Prosthesis: Immediate or delayed temporary teeth to guide soft tissue healing.
Osseointegration Monitoring: Assess implant stability over 3–6 months.
Final Restoration: Attach custom crown, bridge, or fixed full-arch prosthesis.
Each phase integrates patient feedback to ensure comfort and predictability.
How Long Is the Healing and Osseointegration Period?
Bone Graft Integration: 4–6 months for new bone formation.
Implant Osseointegration: 3–4 months until implant stability thresholds are met.
Combined Protocol (All-on-4): Owing to immediate loading, provisional teeth are placed immediately, with final prosthesis at 3–4 months.
Healing intervals vary by individual health, but careful monitoring ensures optimal integration.
How Is Post-Operative Care Managed to Ensure Success?
Soft diet and cold compresses in the first 48 hours
Gentle oral rinses and prescribed antibiotics to prevent infection
Scheduled check-ups to track healing and adjust temporary restorations
Transition to regular oral hygiene once soft tissue healing is complete
Consistent follow-up and clear instructions support comfort and implant longevity.
How Can You Schedule a Consultation for Bone Grafting and Implant Options at Tulsa Time Dental Design?
What Information Should You Prepare for Your Implant Assessment?
Gather your dental and medical history, a list of current medications, and any recent imaging records. Be ready to discuss your aesthetic goals, budget considerations, and any anxiety triggers.
How Does Tulsa Time Dental Design Facilitate Easy Appointment Scheduling?
Our office offers online booking, direct phone access, and prompt assistance from a dedicated patient coordinator. Evening and weekend slots accommodate busy schedules, ensuring you find a convenient time for consultation.
What Do Local Patients Say About Their Implant and Bone Grafting Experiences?
Patients praise the practice for compassionate care, clear communication, and predictable results. Testimonials highlight relief from anxiety, efficient treatment timelines, and restored confidence in eating, speaking, and smiling.
Choose The Right Implant for You
Choosing the right implant path depends on bone health, treatment goals, and personal comfort. Whether you pursue traditional implants with grafting or opt for the streamlined All-on-4 protocol, Tulsa Time Dental Design stands ready to guide you through every phase. Let us help you reclaim function and confidence—schedule your personalized consultation today.
Missing teeth no longer define your quality of life when expert guidance, advanced diagnostics, and compassionate care combine to deliver lasting results. At Tulsa Time Dental Design, we tailor implant solutions to your bone health and lifestyle, ensuring you smile with confidence from day one.